Clinical record
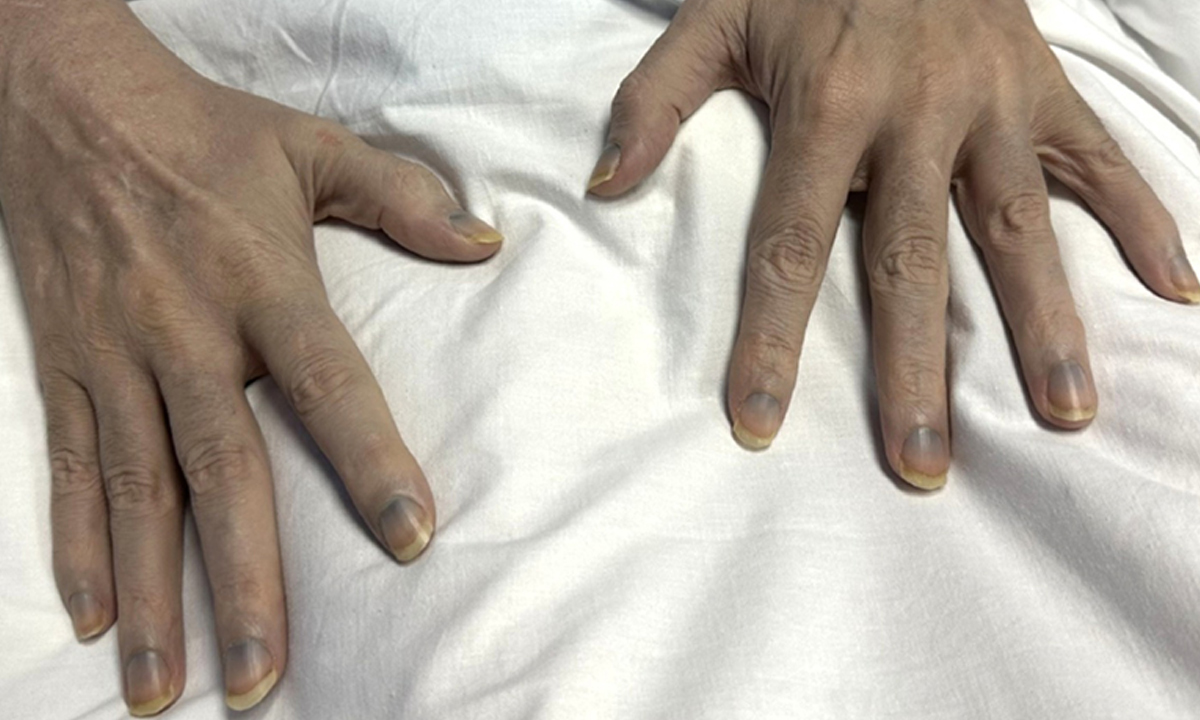
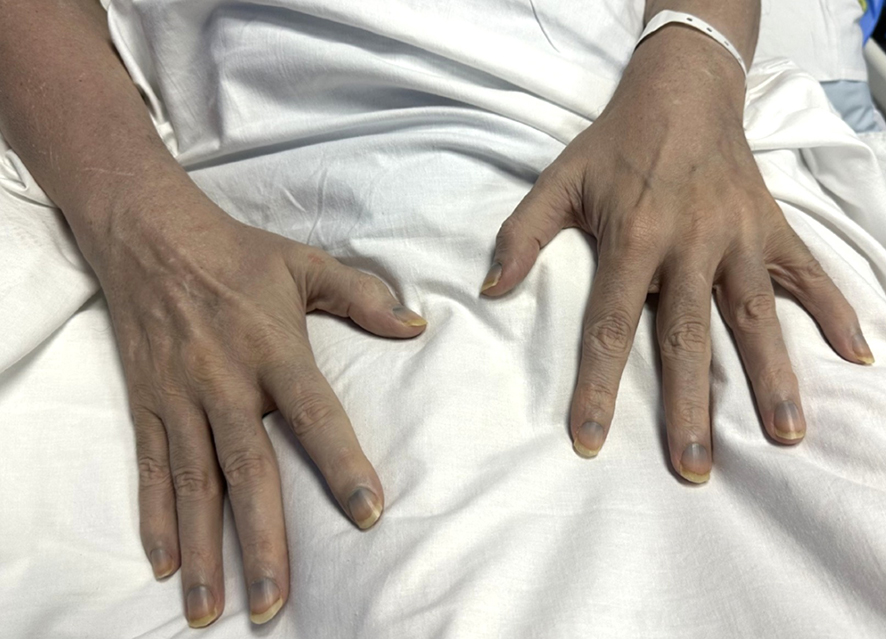
A 63‐year‐old man was brought to the emergency department after a fall with prolonged floor lie of two days, complicated by urinary retention and acute kidney injury, in the context of peripheral neuropathy. His medical history was limited to chronic fatigue syndrome, and he seldom sought medical care. He took no prescribed medications. Examination revealed blue‐grey skin discolouration, most prominent on the sun‐exposed areas of the face and neck. His fingernails showed grey pigmentation extending from the lunulae up the nail (Box 1). No other mucocutaneous abnormalities or organomegaly were noted.
Further discussion revealed that the patient had been using a homemade silver solution to treat a flu‐like illness during the coronavirus disease 2019 (COVID‐19) pandemic, as he had read online claims about the antiviral properties of silver. He stopped using the homemade solution after two months; however, he continued applying commercially available colloidal silver ointment to his legs for two years. He could not quantify his total silver consumption.
The peripheral neuropathy was attributed to type 2 diabetes mellitus, confirmed with elevated HbA1c levels; however, contribution from silver toxicity could not be excluded. Nerve conduction studies confirmed a length‐dependent axonal sensorimotor polyneuropathy. His renal function gradually normalised. Investigations revealed a serum silver concentration of 297 nmol/L (reference interval, < 3 nmol/L) and 24‐hour urinary silver excretion of 227 nmol/24 h (reference interval, < 15 nmol/24 h). A diagnosis of argyria was made clinically (see Box 2 for differential diagnosis). The patient declined a confirmatory skin biopsy. He was advised to discontinue silver use, and after two months of cessation, there was no noticeable change in skin discolouration. No additional complications of argyria were identified. He expressed a desire to resume silver use.
Discussion
Argyria is a rare but striking condition of skin pigmentation resulting from prolonged exposure to silver. Occupational silver exposure may occur in industries such as mining and jewellery‐making, although intentional consumption of colloidal silver has been an increasing concern.1,2,3 Silver accumulates in tissues, leading to characteristic blue‐grey discolouration, exacerbated by sunlight, which catalyses the reduction of silver salts and stimulates reactive melanocyte activity.1,2 Deposited silver granules are inert and not responsive to chelating agents.4,5 Although argyria is not life‐threatening, it is largely irreversible, and no highly efficacious treatment options exist.6 There is emerging evidence that laser therapy may be an effective treatment; however, it is unlikely to fully reverse discolouration.6 Affected individuals should be encouraged to stop using silver‐containing products and minimise sun exposure to prevent further aggravation of the condition. Other reported complications include renal, hepatic and neurological toxicity, although these are rare.2,3 Peripheral neuropathy has been linked to silver toxicity, although causality is usually difficult to establish.7 Case reports suggest that silver excretion can be prolonged, with elevated serum levels persisting for years after discontinuation.5
This case exemplifies the dangers of unverified health remedies, particularly when driven by internet misinformation. Public health crises, such as the COVID‐19 pandemic, foster an environment ripe for the spread of misinformation across internet platforms and social media.8,9 For many years, alternative therapies such as colloidal silver have been readily promoted online for their alleged health benefits despite lacking evidence of efficacy or safety.3 Colloidal silver products sold in major online retailers brazenly claim to eliminate bodily toxins and defend against viruses.3 False marketing claims and the widespread availability of silver products have raised concerns internationally, prompting regulatory agencies, including the United States Food and Drug Administration, to caution against their use.3
In Australia, over two‐thirds of the population report using alternative and complementary medicine products, with more than half failing to inform their health care providers.10 One in eight medicines is purchased without medical advice, while a comparable number are used based on recommendations from friends or media.11 The largest uptake of complementary medicines in Australia is among younger individuals under 35 years, who are tertiary‐educated and female‐identifying, although people with chronic diseases, including cancer and mental illness, also frequently use alternative therapies.10,12 Despite attempts to regulate herbal products by the Australian Register of Therapeutic Goods, these products are exempt from rigorous efficacy assessment and rely on manufacturer self‐evaluation. Previous review has highlighted significant non‐compliance with these regulations in terms of formulation and quality.12 Regulatory oversight does not extend to imported products for personal use. Unfortunately, this limited regulation may give a false sense of safety to consumers.
In an era where misinformation is widely and freely accessible, health care providers must be increasingly alert to the rising use of complementary and alternative medicines. Clinicians must stay proactive and informed in helping patients navigate the abundance of potentially harmful alternative therapies and be willing to foster open communication around their use and safety.
Lessons from practice
- Argyria is a rare but permanent condition caused by prolonged silver exposure, often linked to consumption of colloidal silver products.
- Early recognition of argyria and cessation of exposure is important to prevent further skin pigmentation or other complications.
- Complementary and alternative health remedies are widespread in Australia although patients may not immediately disclose their use.
- Health misinformation can have harmful consequences thus clinicians should engage patients in open communication about alternative medicines and advise them appropriately on the potential dangers.
Box 1 – Agyria: discoloration of the hands and nail beds
Box 2 – Differential diagnosis of generalised argyria or skin discolouration
|
Condition |
Detail |
||||||||||||||
|
|
|||||||||||||||
|
Drug‐induced hyperpigmentation |
Often affects sun‐exposed skin. The following may cause blue‐grey discolouration:
|
||||||||||||||
|
Diffuse melanosis cutis |
Progressive pigmentation over weeks to months, seen in metastatic melanoma4 |
||||||||||||||
|
Cyanosis |
Related to hypoxia or altered haemoglobin states as in methaemoglobinaemia13 |
||||||||||||||
|
Metabolic disorders (causative agent; skin change) |
|
||||||||||||||
|
Other heavy metal exposures |
|
||||||||||||||
|
|
|||||||||||||||
|
|
|||||||||||||||
link